Breast Cancer Doesn't Grow in a Healthy Neighborhood (Part 2)
The Terrain, Mitochondria, and What Most Oncology Visits Miss (Part 2)
By: Jill Chmielewski, May 15, 2026
In Part 1, I walked you through the other pathways that drive breast cancer growth: PI3K/AKT/mTOR, MAPK, androgen, JAK-STAT, EGFR, Notch, Wnt, Hippo, and the stem cell pathways. The takeaway was simple but rarely said out loud. Breast cancer is not a hormone problem. It's a many-pathway problem. And most of the conversation women are handed centers almost entirely on estrogen.
Today I want to zoom out even further.
Because here's the truth I keep coming back to in my work. Cancer cells don't just go rogue. They don't drop out of the sky. A cancer cell is a cell that finally couldn't keep up. It couldn't repair itself, couldn't make enough energy, couldn't keep its signaling clean. And it lived in a body that, for many reasons, had stopped being a healthy place to live.
That's what I want to talk about. The neighborhood. The terrain.
The Cancer-in-the-Neighborhood Analogy
Imagine a quiet neighborhood.
Lawns mowed. Streetlights working. Garbage is picked up on Tuesdays. Neighbors checking on each other. Police and fire arrive quickly when something goes wrong.
In a neighborhood like that, a single rough house can usually be cleaned up before it becomes a problem.
Now picture a different neighborhood.
The streetlights are out. Trash piles up. Nobody fixes anything. The fire trucks don't come. The police are stretched thin. A single broken window doesn't get repaired. It becomes ten broken windows, then a vacant building, then a whole block in trouble.
That second neighborhood is the terrain where most cancers grow.
The cancer cell itself is real. The mutations are real. But the question I want women to start asking is the one almost no oncology visit gets to: why is the neighborhood letting this happen? What stopped working? What was missing? What was there in excess? What was the body trying to tell us long before a tumor showed up?
This is the terrain question. And it's the question almost every functional medicine and integrative oncology framework starts with.
Cancer Is Not Just a Genetic Disease. It's a Metabolic One.
Almost a century ago, a German researcher named Otto Warburg noticed something strange. Cancer cells, even when there is plenty of oxygen around, prefer to burn sugar in a sloppy, inefficient way. They skip the part of the cell that should make clean energy (the mitochondria) and ferment glucose instead. He called this aerobic glycolysis. We now call it the Warburg effect.[1, 2]
Here is why that matters.
Your mitochondria are the tiny power plants inside almost every cell of your body. They convert food and oxygen into ATP (adenosine triphosphate), the molecule your cells run on. Every heartbeat, every thought, every breath is powered by mitochondrial ATP.
Mitochondria also act like cellular smoke detectors.
They monitor oxygen levels, nutrient availability, oxidative stress, infection signals, and DNA damage. When something is off, they release signals (like cytochrome c, mitochondrial DNA fragments, and reactive oxygen species) that tell the rest of the cell and the immune system that there's a problem. They decide when a damaged cell should repair itself, and when it should quietly self-destruct (a process called apoptosis). Healthy mitochondria are how the body cleans up problem cells before they become tumors.
When mitochondria stop working well, three things happen at once.
Cells start running on the cheap, dirty fuel pathway (the Warburg effect).
Damaged cells stop self-destructing on schedule.
The body loses one of its most important cancer-prevention systems.
A growing body of research, including the work of researcher Thomas Seyfried, argues that cancer is at its heart a disease of broken mitochondria and metabolic chaos.[3, 4] The genetic mutations we see in tumors? Many of them appear to be downstream consequences of mitochondrial dysfunction, not the original cause.[5]
This doesn't mean genes don't matter. They do. But it reframes the question. Instead of asking what mutation caused this cancer, we start asking what damaged the mitochondria so badly that the cell couldn't keep up?
And once you start asking that question, the list of things to look at gets very long. And very fixable.
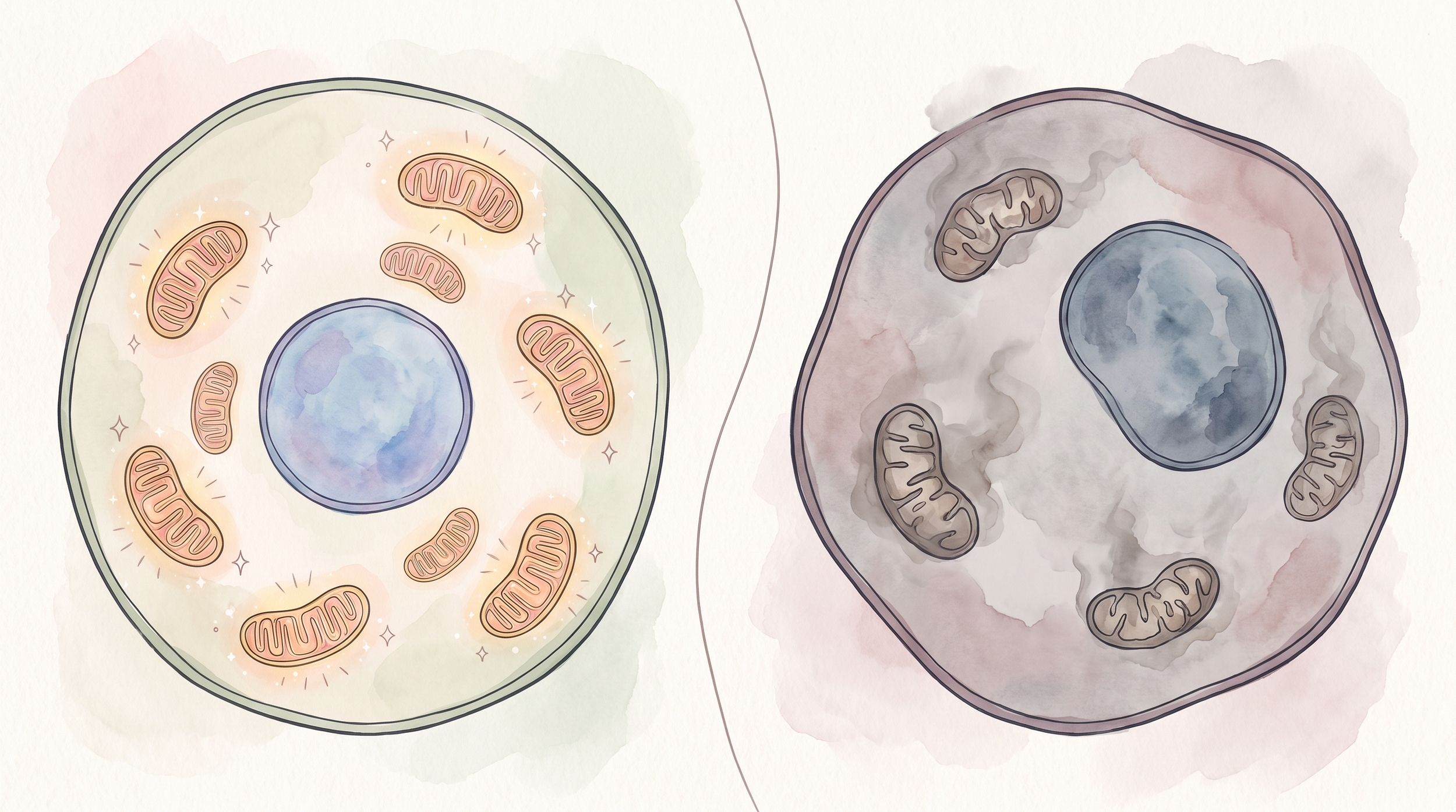
On the left, the healthy cell has plump, glowing peach-pink mitochondria with neat folded cristae and little sparkle marks suggesting clean energy. On the right, the cancer cell is irregular, dusty grey-mauve, with fewer, dimmer mitochondria, faded cristae, and a hazy murky cytoplasm.
What Damages the Terrain
Mitochondria are sensitive little things. They don't like a lot of what modern life serves up. They get damaged by:
Chronic blood sugar swings and insulin resistance
Ultra-processed food, seed oils, and refined sugar
Environmental toxins — pesticides, plastics, heavy metals, indoor air pollution
Chronic stress and elevated cortisol
Poor sleep, especially over years
Sedentary living
Chronic, low-grade infections (Epstein-Barr, gum disease, gut dysbiosis, mold, Lyme)
Nutrient deficiencies (especially B vitamins, magnesium, CoQ10, vitamin D, omega-3s)
Loss of hormonal signaling at menopause — estrogen, progesterone, testosterone, DHEA, and thyroid all support mitochondrial function in different ways
Trauma — yes, the body keeps the score, and unresolved emotional stress is a real biological hit
When you see that list, you start to understand why so many women in midlife feel like everything went sideways at once. The terrain has been quietly degrading for years. Menopause, with its sharp drop in protective hormones, just pulls back the curtain.
The good news is that almost every item on that list is something you can do something about.
The "Maximize, Minimize, Prioritize" Checklist
This is the framework I learned in my functional medicine training and the one I’ve used with women in my own practice. It’s called Optimal Health Simplified, which lays it out in full. Here is the heart of it.
Healing the terrain comes down to three questions.
1. What does my body need MORE of?
These are the inputs the body needs to function well, repair itself, and clean up before things go wrong.
Oxygen and clean air — most women are mouth-breathing, shallow-breathing, or sitting indoors all day
Clean water
Vitamins, minerals, and antioxidants from real food
Healthy fats — olive oil, avocado, pastured butter, fatty fish
Fiber — from a wide variety of plants
Protein — most women in midlife are eating far too little
Slow, mindful eating — digestion starts before the first bite
Balanced hormones — when appropriate, this includes hormone treatment
The right kind of exercise — strength training, walking, zone 2 cardio, not endless punishing cardio
Sunlight — especially morning sun, on your skin and in your eyes
2. What does my body need LESS of?
These are the things that drain the terrain and damage the mitochondria.
Toxins — household cleaners, fragrances, plastics, pesticides
Stressful relationships and unprocessed trauma
Chronic infections — including hidden ones
Allergens and sensitivities the body is fighting in the background
Stress — the chronic, never-shuts-off kind
Screen time and social media doom loops
Ultra-processed food and refined sugar
Late nights and disrupted sleep
Limiting beliefs, fear, and negative thinking — these are not soft. They change biology.
3. What does my body need to PRIORITIZE so it can heal?
This is the part most women skip. Healing doesn't happen in a body that never gets to rest, breathe, laugh, or be still. And it’s important to remember that your body cannot heal in the same environment that made you sick.
Sleep and rest
Laughter and play
Stress management — meditation, breathwork, prayer, walking, swimming
Time to prepare and eat real food
Time in nature
Breathing — slow, through the nose
Meaningful relationships
Purpose and passion
When women ask me where to start, this is where I send them. Not to a single supplement. Not to a magic protocol. To this checklist. Because the body knows how to heal. It just needs the right conditions.
A Question Worth Asking: COVID, Spike Protein, and p53
This part is going to feel different from the rest, and I want to walk into it carefully.
One of the body's most important cancer-prevention tools is a protein called p53. It is sometimes called the "guardian of the genome" because its job is to spot damaged cells and either repair them or quietly trigger their self-destruction. A working p53 is one of the reasons most early cell damage never becomes cancer.
p53 and the SARS-CoV-2 Spike Protein
In the last few years, peer-reviewed research from Brown University and Lifespan Health System has shown that the SARS-CoV-2 spike protein (the same protein produced by COVID infection and by the mRNA vaccines) can interfere with p53's job. In their experiments, cancer cells expressing spike protein had reduced p53 activity, were less able to die when exposed to chemotherapy, and showed signs of impaired DNA damage response.[6]
Other published work has explored how repeated spike protein exposure may also drive cell senescence, inflammation, and a kind of long-tail biological stress that may matter for cancer risk.[7] Think of cell senescence as a cell going into "retirement mode,” but a bad kind of retirement, where the cell refuses to leave the building. The worst part about these retired cells is that they start leaking inflammatory chemicals into the surrounding tissue
That inflammatory leak has a name: SASP (Senescence-Associated Secretory Phenotype).
It's a stew of inflammatory signals, growth factors, and tissue-damaging enzymes that irritates neighboring healthy cells and can actually turn them senescent too. Scientists call these cells "zombie cells" because they're not alive in a useful way, not dead, and they're contagious. It’s not a good situation.
The menopause connection
Estrogen helps keep senescence in check. When estrogen drops in perimenopause and menopause, senescent cells accumulate faster, which is part of why so many "aging" symptoms seem to hit all at once in midlife. It's not just hormone loss; it's hormone loss plus a sudden buildup of zombie cells driving inflammation. Researchers are working on senolytics, drugs and compounds that selectively kill senescent cells while leaving healthy ones alone. Some natural compounds being studied include quercetin, fisetin, and curcumin. Early animal studies show that clearing senescent cells can reverse some signs of aging.
I am not telling you what to do with that information.
I am telling you it exists, it is published in legitimate journals, and it is a fair question to bring up with your clinician, especially if you have a personal or family history of breast cancer, or known BRCA or p53 changes.
If you want to know whether spike protein is still circulating in your body, there are labs offering spike protein testing. This is something to ask an integrative or functional medicine clinician about. It is not a routine oncology test, but it is becoming more available.
This is not about fear. It is about asking the same question we are asking everywhere else: what may have shifted the terrain? And being willing to look at every reasonable possibility.
About Aromatase Inhibitors and Tamoxifen — The Cost Almost No One Talks About
I want to be honest here, because women deserve the whole picture.
Aromatase inhibitors (drugs like anastrozole, letrozole, and exemestane) and tamoxifen are the most common drugs prescribed after an estrogen-receptor-positive breast cancer diagnosis. They can reduce recurrence risk in some women. That is real, and it matters.
But the conversation almost always stops there. What women are rarely told is what these drugs cost the rest of the body.
Aromatase inhibitors essentially block estrogen everywhere
Aromatase is the enzyme that lets your body make estrogen from other hormones. Before menopause it works mostly in your ovaries. After menopause it works in your fat, bone, brain, and other tissues. After menopause, this peripheral aromatase activity is essentially your only source of estrogen. An aromatase inhibitor turns that source off, body-wide.
Estrogen is not just a reproductive hormone. It is a signaling molecule for almost every system in the body. When you take it away everywhere, the downstream effects are significant. Published reviews on aromatase inhibitor toxicity describe:[8]
Bone loss and fracture risk — estrogen is one of the strongest signals to keep your bones building rather than dissolving
Joint pain and stiffness — sometimes severe enough that women stop the drug
Muscle loss and sarcopenia
Vaginal dryness, painful sex, and recurrent urinary infections (genitourinary syndrome of menopause)
Hot flashes and night sweats
Mood changes, anxiety, and depression
Sleep disruption
Cognitive complaints — the foggy, slow, lost-words feeling
Cardiovascular shifts — changes in cholesterol and blood pressure
Metabolic changes — insulin resistance, weight gain, body composition shifts
Hair thinning and skin changes
Increased risk of autoimmune flares — estrogen helps regulate the immune system
Some of these effects can be managed. Many cannot, because the underlying issue is no estrogen anywhere, and there is no good substitute for what estrogen does in tissues that aren't the breast.
Tamoxifen works differently but has its own costs
Tamoxifen is a selective estrogen receptor modulator. It blocks estrogen in some tissues (breast) and acts like estrogen in others (bone, uterus, liver). Its known effects include:
Hot flashes, night sweats, and mood changes
Increased risk of blood clots and stroke
Increased risk of endometrial cancer
Cataracts
Cognitive effects
Fatty liver and changes in liver enzymes
This is not me telling you to stop your medication. This is me saying: know what you are signing up for. Ask what monitoring is in place. Ask what can be done to protect your bones, your brain, your joints, and your heart. Ask whether all of these costs can be addressed. (Spoiler: not all of them can.)
And ask the harder question. “If estrogen does this much work in the body, and we know that women without estrogen signaling have higher rates of osteoporosis, dementia, cardiovascular disease, and autoimmune flares, what are we actually trading?”
Women deserve to ask that question. Out loud. Without being told they are difficult.
Where Repurposed Drugs Fit In
I touched on this briefly at the end of Part 1, and it belongs here too.
If cancer is a multi-pathway, metabolic, terrain disease, then it makes sense that some of the most promising research is looking at older, well-studied drugs that quietly hit those terrain-level pathways.
Drugs like metformin (mitochondrial function and insulin signaling), mebendazole (cancer stem cells and mitochondria), ivermectin (multiple pathways), doxycycline (cancer stem cells via mitochondrial inhibition), and propranolol (stress signaling). Plus nutraceuticals like curcumin, resveratrol, vitamin D, melatonin, and berberine.
Dr. Paul Marik and theIndependent Medical Alliance have put together a Cancer Care guide that walks through this work in detail. The framing is not anti-conventional care. It is and-also. What if the standard treatment is one piece of the puzzle, and the rest of the puzzle is supporting the terrain (mitochondria, metabolism, immune function) at the same time?
This is the conversation an integrative oncologist or functional medicine clinician can have with you. Most conventional oncology visits do not have time for it. That is not a criticism. It is just the reality of how the system is set up.
So, Where Does That Leave You?
I want to leave you with hope, because hope is the part of this story that gets stripped away by a system that talks only about tumor staging and drug regimens.
Here is what I want you to take with you.
Cancer is not random. It does not just happen to you out of nowhere. Something shifted in the terrain. And that something is often a long list of things, accumulated over years, that pushed the body past what it could repair on its own.
Your body knows how to heal. It does this every minute of every day. Damaged cells get repaired or removed. New cells get built. Energy gets made. Inflammation gets resolved. The whole system runs on what you give it and what you take away.
You do not have to fix everything at once. Pick one thing on the Maximize list. Pick one thing on the Minimize list. Pick one thing on the Prioritize list. Do those for a month. Then add the next layer.
You are allowed to ask hard questions about every recommendation you receive. What does this drug do everywhere in my body? What is the absolute risk reduction, not just the relative one? What is being monitored? What is being missed? What else could I be doing alongside this?
You are allowed to build a team that looks at the whole picture. An oncologist for the cancer-specific decisions. An integrative oncologist or functional medicine clinician for the terrain. A pelvic floor physical therapist. A nutritionist who actually understands metabolism. A therapist for the emotional layer. A friend who reminds you that you are not your diagnosis.
You are still you. A diagnosis does not change who you are. It changes some of the decisions you have to make. That is all.
The most powerful thing I can say to a woman walking through this is: your body is wise. Partner with her. Partner with the right people. And keep asking the question that almost no one will ask for you.Why is this happening in this body, in this neighborhood, right now?
That question is the beginning of healing.
For more information on this topic, see my other articles:
Hormones & Breast Cancer: What’s Fact, What’s Fiction?
The History of Breast Cancer Treatments and the Misguided War on Estrogen
The Truth About Estrogen, Breast Cancer, and Hormone Therapy: What the Latest Research Reveals
Check out the Breast Cancer Series in the Balance App
References
1. Seyfried, T. N., Lee, D. C., Duraj, T., Ta, N. L., Mukherjee, P., Kiebish, M., Arismendi-Morillo, G., & Chinopoulos, C. (2025). The Warburg hypothesis and the emergence of the mitochondrial metabolic theory of cancer. Journal of Bioenergetics and Biomembranes, 57(2–3), 57–83. https://doi.org/10.1007/s10863-025-10059-w
2. Jiang, H., & Ye, J. (2025). The Warburg effect: The hacked mitochondrial-nuclear communication in cancer. Seminars in Cancer Biology, 112, 93–111. https://doi.org/10.1016/j.semcancer.2025.03.006
3. Seyfried, T. N., Yu, G., Maroon, J. C., & D'Agostino, D. P. (2017). Press-pulse: a novel therapeutic strategy for the metabolic management of cancer. Nutrition & Metabolism, 14(1), 19. https://doi.org/10.1186/s12986-017-0178-2
4. Seyfried, T. N., Mukherjee, P., Iyikesici, M. S., Slocum, A., Kalamian, M., Spinosa, J.-P., & Chinopoulos, C. (2020). Consideration of Ketogenic Metabolic Therapy as a Complementary or Alternative Approach for Managing Breast Cancer. Frontiers in Nutrition, 7, 21. https://doi.org/10.3389/fnut.2020.00021
5. Seyfried, T. N., & Chinopoulos, C. (2021). Can the Mitochondrial Metabolic Theory Explain Better the Origin and Management of Cancer than Can the Somatic Mutation Theory? Metabolites, 11(9), 572. https://doi.org/10.3390/metabo11090572
6. Zhang, S., & El-Deiry, W. S. (2024). Transfected SARS-CoV-2 spike DNA for mammalian cell expression inhibits p53 activation of p21(WAF1), TRAIL Death Receptor DR5 and MDM2 proteins in cancer cells and increases cancer cell viability after chemotherapy exposure. Oncotarget, 15(1), 275–284. https://doi.org/10.18632/oncotarget.28582
7. Kyriakopoulos, A. M., Nigh, G., McCullough, P. A., & Seneff, S. (2022). Mitogen Activated Protein Kinase (MAPK) Activation, p53, and Autophagy Inhibition Characterize the Severe Acute Respiratory Syndrome Coronavirus 2 (SARS-CoV-2) Spike Protein Induced Neurotoxicity. Cureus, 14(12), e32361. https://doi.org/10.7759/cureus.32361
8. Nardin, S., Ruffilli, B., Landolfo, T. L., Isingrini, G., Taglialatela, I., Delbarba, A., D'Avanzo, F., Rossi, V., Celentano, E., Conte, B., Nardin, M., & Gennari, A. (2025). Aromatase Inhibitors as Adjuvant Therapy in Early Breast Cancer: Insights into Toxicities and Their Management. Cancers, 17(17), 2726. https://doi.org/10.3390/cancers17172726
Disclaimer: This article is for educational and informational purposes only and is not intended to replace personalized medical advice or individualized care. It is meant to help you understand your physiology, explore evidence-based options, and make informed choices about your health and wellness. Healthcare should be a partnership, not a permission slip, and proactive care is just as essential as treatment. Use this information to engage in open, collaborative discussions with your provider or to make empowered decisions that align with your own values, goals, and comfort level. You are the ultimate authority on your body.